Dental Therapy
For the prevention of caries, proper daily oral hygiene at home is important, carried out with the aid of a toothbrush, toothpaste and dental floss. A useful support can be constituted by professional oral hygiene at the dentist, who can make use of the collaboration of a dental hygienist.


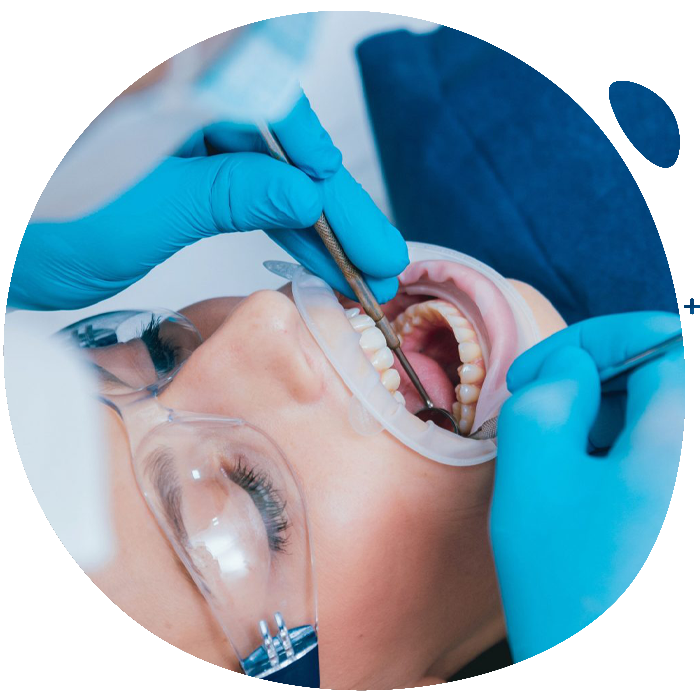
What is dental
therapy?
Tooth decay is a degenerative disease of the hard tissues of the tooth (enamel, dentine) on a bacterial basis, which originates from the surface and continues to the dental pulp. Its causes are the usual microorganisms present in the oral cavity, mainly those that stick to the tooth in the form of bacterial plaque, which if not kept under control through usual oral hygiene practices, or in the case of reduced immune protection, are able to break down the mineral and organic matrix that makes up the tooth, creating cavitated lesions. The main symptom is pain, which, however, often appears only when the process has gone too deep, affecting the organ of the pulp (pulpitis). Treatment includes removing the infected tissue and replacing it with suitable material (conservative dentistry) and, in case of advanced pulp involvement, removing the pulp tissue and replacing it (endodontics).
Fluoride
Fluoride has the ability to remineralize tooth enamel, block the metabolic pathways of bacteria responsible for caries (bacterial enolase) and reduce bacterial adhesion to tooth surfaces. S. mutans produces lipoteic acid, which attaches to the resulting film by means of a calcium ion Ca ++ . Fluoride, which replaces the Ca ++ ion, inhibits bacterial adhesion, but special attention should be paid to the use of this element, as it is found in many products for oral hygiene, chewing gum, anesthetics, psychotropic drugs and others. like. as well as obviously in nature; if taken carelessly in the first years of life (at puberty), in fact, it is possible to create a fluorosis, with the risk of damage to the teeth, bones and nervous system. Fluorosis appears if during the histogenesis of hard tooth tissues (up to 12 years), fluoride intake exceeds 2 mg. For obtaining this element, it is advisable to always consult a dentist or doctor.
Sealing
Dental bonding has been proven to be a useful primary prevention practice. It is performed through the preventive filling of the grooves and dimples located on the occlusal surfaces of the teeth with a special material, usually not long after their emergence, to prevent bacterial colonization and consequently the development of carious pathology.
Some foods have proven activity against some bacteria of the oral cavity and in particular against Streptococcus mutans: xylitol, proanthocyanins darkoni (red wine, blueberry, cinnamon), tea tree oil, curcuminoid, green tea rich in catechins, barley drink. , fluoride, chlorhexidine, some flavonoids present in the white peel of citrus peel, glycyrrhizic acid A present in licorice sticks (if swallowed in the mouth for more than 4-5 minutes).
A group of researchers would have identified substances in red wine that can neutralize the attack of Streptococcus mutans on tooth enamel. This is most likely a group of compounds known as proanthocyanidins. The practical utility of this discovery, however, appears to be questionable.
Gum therapy
Gingivitis consists of inflammation of the gums: it is a simple solution to gingival discomfort, which should not be underestimated, however, since neglected gingivitis can be the beginning of real pathologies, such as pyorrhea (or periodontitis) . Prevention is essential, therefore careful daily oral hygiene accompanied by frequent dental check-ups.
Causes
The causes of gingivitis basically lie in the accumulation of plaque on the surface of the teeth and gums: plaque is a sticky and opalescent film, an ideal breeding ground for bacteria. The risk of contracting gingivitis increases in case of pregnancy, diabetes, smoking, alcohol abuse, excessive intake of corticosteroids and antidepressants, neglect of dental hygiene and genetic predisposition.
Vitamin deficiency can also promote oral inflammation, creating gingivitis.
Symptoms
In the early stages, gingivitis begins with mild irritation and inflammation of the gums, which tend to bleed during brushing. The patient suffering from gingivitis often complains of halitosis, which becomes more pronounced in relation to the severity of the disease. Neglected gingivitis degenerates into pyorrhea, thereby exponentially increasing the risk of tooth loss.
Information on gingivitis – gingivitis medications is not intended to replace the direct relationship between the healthcare professional and the patient. Always consult your doctor and/or specialist before taking Gingivitis – Medicines for the treatment of gingivitis.
Drugs
In the initial stage, gingivitis is easily reversible; however, when neglected, gum inflammation is prolonged creating more and more damage. Given the ease of solving gingivitis at its onset and the difficulty of healing when it is neglected, it is necessary to emphasize once again the importance of daily oral hygiene, which must be repeated at least three times a day, and periodic checks from the dentist.
Dental hygiene treatment at home includes:
- brush your teeth at least three times a day, with specific toothpaste
- floss at least once a day
- use an antiseptic mouthwash
Professional dental hygiene consists of:
- dental cleaning aimed at removing plaque and tartar
- repeat cleaning twice a year
Pharmacological treatment for the treatment of gingivitis includes taking pharmacological formulations based on bactericides and anti-inflammatory substances, such as steroids (topical application) and antiseptics (substances with disinfectant action).
Below are the drug classes most commonly used in gingivitis therapy and some examples of pharmacological specialties; It is up to the doctor to choose the active ingredient and the most suitable dose for the patient, based on the severity of the disease, the patient’s state of health and his response to treatment:
Hydrocortisone
(eg Cortison CHEM, Idroco A ECB): this medication belongs to the class of corticosteroids: in case of gingivitis it should be applied locally, in the form of a cream or toothpaste. The product is useful for reducing inflammation. It is recommended to apply it directly to the inflamed gums, two or three times a day, after meals and before going to sleep. In general, it is advisable to apply a generous additional dose of the drug without allowing it to be absorbed, in order to create a kind of protective film on the surface of the tooth. If there is no improvement after 7 days of therapy, a change of drug is recommended. Hydrocortisone is often found in combination with antibiotics, such as neomycin and polymyxin B (eg Mixoton).
Chlorhexidine
(e.g. disinphene cream, golasan mouthwash): rinse the teeth with 15 ml of the product, twice a day, after brushing well with toothpaste. It is recommended to keep the chlorhexidine-based mouthwash in the mouth for at least 30 seconds before taking it out. The drug is used in the therapy of gingivitis due to its disinfectant and anti-inflammatory properties. Do not swallow mouthwash.



